|
6/21/2023 0 Comments Normal range of capnography 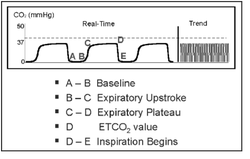
As aerobic metabolism falls and the patient becomes more acidotic, exhaled CO2 will also fall.Ĭapnography is available for both spontaneously breathing patients and patients who are receiving positive pressure ventilation. The same holds true in altered metabolic states such as diabetic ketoacidosis. This increase in exhaled CO2 occurred significantly earlier than palpable pulses or blood pressure. In cardiac arrest, for example, a sharp rise in EtCO2 was determined to be the earliest indicator of return of spontaneous circulation (ROSC) in two prehospital studies. There is a large volume of data suggesting that failure to achieve an end-tidal CO2 above 10 mmHg within the first 20 minutes of CPR is never associated with ROSC (return of spontaneous circulation) and could reasonably be used to terminate resuscitation.įinally, capnography reflects metabolism, and seems to be one of the earliest indicators of alterations in metabolic activity. An EtCO2 of less than 10 mmHg during an arrest suggests that the chest compressions are not deep or fast enough, that the rescuer is tired (hence the reason we need to change compressor every two minutes), or that excellent CPR is not producing even minimal perfusion. Nowhere is this more powerfully illustrated than during CPR. If perfusion declines for any reason, such as a drop in cardiac output or the onset of a shock state, the amount of CO2 being returned to the lungs will fall. In a steady state, CO2 production remains relatively consistent, hence measuring exhaled CO2 directly reflects ventilation. Simply, our bodies use oxygen and water to make energy carbon dioxide is the waste product of that process. Understanding the meaning and value of capnography begins with an appreciation of how carbon dioxide is generated in the body. Available for both intubated and spontaneously breathing patients, and now a part of the EMT curriculum, capnography is an amazingly valuable tool and one you can most certainly rely on. While pulse oximetry mirrors oxygenation status, capnography reflects ventilation, perfusion, and metabolism. and is now becoming a standard of care in EMS, the emergency department and the ICU. During the 1980s, capnography became a standard for anesthesia care in the U.S. Capnography is the non-invasive measurement of exhaled carbon dioxide (CO2) displayed as a CO2 waveform concentration over time. In the life and death business of EMS, you need tools that you can rely upon. October 3rd, 2018 CapnoAcademy Articles, Capnography 101, Columnistsįor both intubated and non-intubated patients, capnography can provide a wealth of information about vital signs Hypocapnia/Hyperventilation 2 An ETCO₂ level lower than normal, less than 4.0 % (34 mmHg), is called hypocapnia.Capnography 101 The critical role of capnography Kalenda, Mastering Infrared Capnography, p48, 1989 Spontaneous breathing can be instituted more easily by allowing the EtCO 2 rise at the end of the anesthesia and patient usually experiences a more rapid recovery.ĭuring lengthy anesthesia, there is typically a very gradual decrease in EtCO 2 due to the depressant effect of anesthetic agents and the effect of hypothermia slowing the patient’s metabolism.ġ Z. 
With normoventilation, disturbances in ventilation, circulation and metabolism can be more easily recognized and monitoring enables to maintain the physiologically optimal minute ventilation. ”carbia” refers to CO 2 level in the bloodĪlveolar minute ventilation is usually adjusted to achieve normocapnia, where EtCO 2 is in the range 4.0-6. 
Hypercapnia EtCO 2 more than 6.0 vol % 45 mmHg Common terms in CO 2 monitoring: Hypocapnia EtCO 2 less than 4.0 vol % 35 mmHg 
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
